Primary Care
We offer comprehensive primary care services focused on prevention, early detection, and management of both acute and chronic conditions. From routine physicals and preventive screenings to the treatment of complex medical concerns, our approach emphasizes personalized, evidence-based care tailored to each patient. Dr. Oza is committed to integrating the latest medical research into everyday practice, helping patients optimize their health and reduce long-term risk. With in-house Gastroenterology, Allergy, and Immunology services, we are able to provide coordinated, multidisciplinary care, making it easier for patients to access specialty evaluation and treatment when needed. Our proximity to Tufts Medical Center also ensures that any additional referrals, imaging, or diagnostic testing can be arranged efficiently and conveniently.
We assist new patients in obtaining outside medical records, and Dr. Oza carefully reviews these documents prior to your visit. Dr. Oza values clear communication and shared decision-making, taking the time to explain diagnoses, test results, and treatment options so patients feel informed and confident in their care.
In a complex medical landscape, your health requires a central coordinator. While specialists provide expert focus on specific systems, Dr. Oza’s role as your primary care physician is to manage your comprehensive health strategy. He ensures that specialist recommendations—including those from our in-house Allergy and Gastroenterology (GI) departments—are integrated into a cohesive plan, resolve potential clinical conflicts, and advocate for the most effective interventions. Sometimes, the most professional course of action is to allow your body’s natural resilience to lead, but he is always available to guide the process and ensure your health remains on track.
Clinical Access
Effective management begins with a proactive partnership. Select the appropriate clinical entry point:
Comprehensive Health Assessment – A foundational evaluation to map your genetic blueprint and establish your clinical strategy.
Acute Care Visit – Prompt intervention to address and neutralize immediate health concerns.
1. Cardiovascular Health & Genetic Risk Assessment
Cardiovascular health is maintained through long-term surveillance rather than reactive treatment.
Clinical Standards: Management is strictly aligned with AHA/ACC Clinical Practice Guidelines.
Risk Calculation: We utilize the AHA PREVENT™ Cardiovascular Risk Calculator.
Precision Medicine: Incorporating ACC/AHA Cardiovascular Genetics to screen for hereditary risks.
2. Cancer Interception & Genomic Surveillance
Modern oncology has shifted from detection to interception. By utilizing precision genomics and specialized Gastroenterology (GI) expertise, we identify risks at a molecular level.
Gastrointestinal Focus: We prioritize high-yield screenings for colorectal and esophageal cancers, coordinating directly with our GI specialists for advanced diagnostics and surveillance.
Hereditary Assessment: We deploy NCCN Genetic/Familial High-Risk Assessments.
Shared Decision-Making: Consultation regarding prostate cancer screening to ensure care aligns with patient values.
3. Mental Health Integrity
Psychological well-being is fundamental to physical health. We conduct standardized mental health screenings at every preventive encounter.
Standardized Tools: Implementation of PHQ-9 and GAD-7 diagnostic screenings.
Clinical Resources: Pathways are available through NIMH Health Topics.
4. Chronic Disease Management
Managing chronic conditions requires consistent systemic stability via ADA Standards of Care and CDC guidelines.
5. Preventive Care & Annual Evaluations
The annual physical is a strategic review of your health status based on USPSTF A and B Recommendations.
6. Geriatric Care & Medication Safety
Prioritizing independence and preventing polypharmacy-related complications using AGS Clinical Tools.
Medication Review: Utilizing the AGS Beers Criteria® to minimize potentially inappropriate medications.
7. Osteoporosis & Skeletal Health
Skeletal integrity is essential for mobility. We focus on bone density preservation and proactive fracture prevention following BHOF Clinical Guidelines.
Therapeutic Exercise: Recommended Bone-Healthy Movements.
8. Immunological Maintenance & Allergy Integration
Immunizations and immunological health are your defense against evolving environmental threats. Our Allergy department works in tandem with primary care to manage complex immune responses.
Allergy & Immunology: Specialized focus on managing allergic rhinitis, asthma, and immunological sensitivities to optimize your daily environment and respiratory health.
Vaccination Protocols: Aligned with ACIP Vaccine Recommendations.
9. Peri-operative Optimization
Comprehensive pre-surgical medical optimization to ensure the best clinical condition for surgery and recovery.
10. Lifestyle Medicine
Lifestyle choices are a primary modality for disease treatment following American College of Lifestyle Medicine protocols.
11. Sports Medicine & Musculoskeletal Recovery
Functional movement is key to healthspan. We utilize ACSM Clinical Guidelines to restore range of motion.
12. Urgent Care & Acute Symptom Management
Rapid clinical intervention following CDC Respiratory Virus Guidance.
13. Universal Genetic Risk Assessment
Personalizing care via the CDC Office of Genomics.
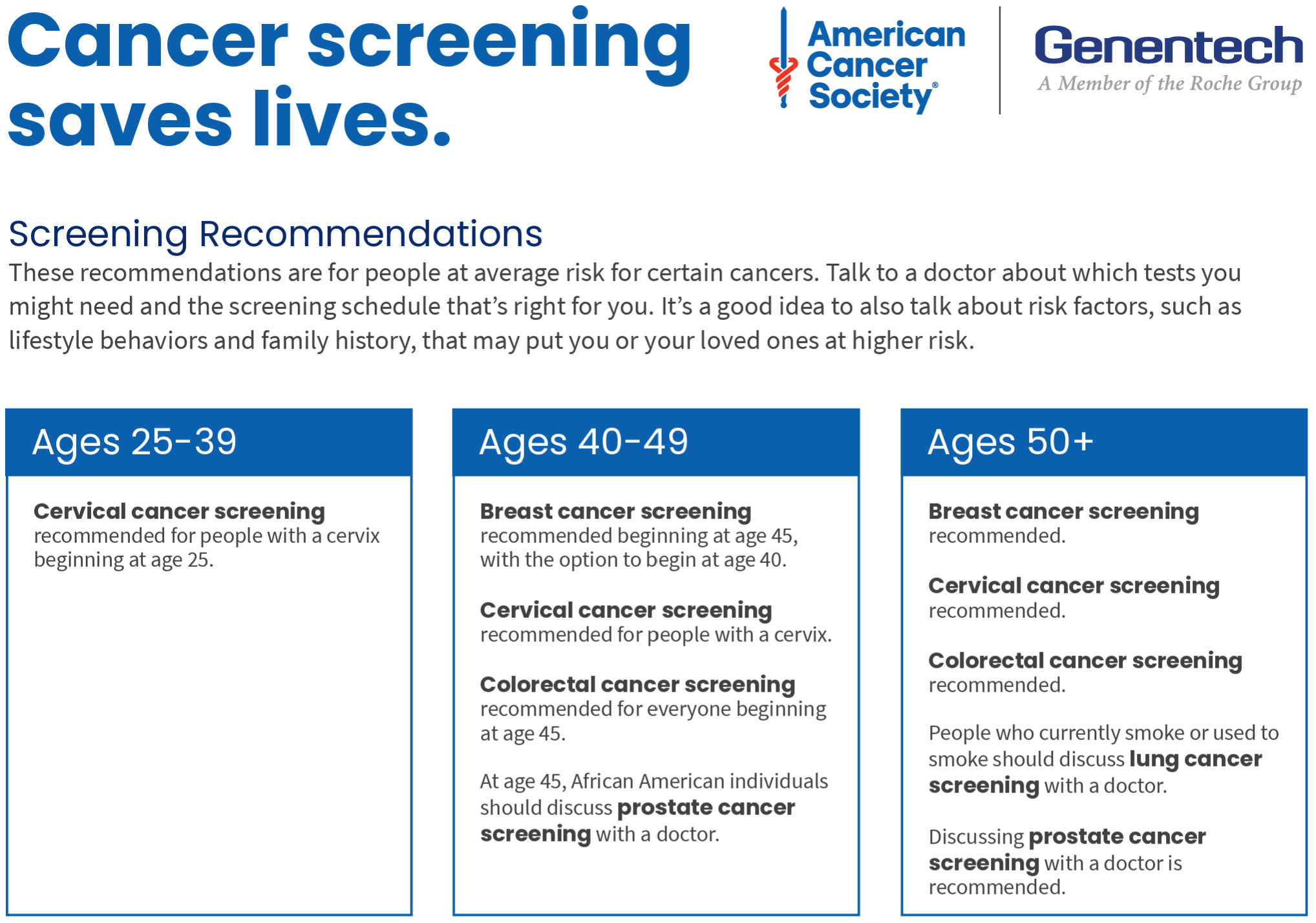
Cancer Screening Schedule
Breast cancer
40-44: should have the choice to start annual breast cancer screening with mammograms (x-rays of the breast) if they wish to do so.
45-54: should get mammograms every year.
55+: should switch to mammograms every 2 years, or can continue yearly screening.
Screening should continue as long as a woman is in good health and is expected to live 10 more years or longer.
All women should be familiar with the known benefits, limitations, and potential harms linked to breast cancer screening.
Women should also know how their breasts normally look and feel and report any breast changes to a health care provider right away.
Some women – because of their family history, a genetic tendency, or certain other factors – should be screened with MRIs along with mammograms.
Cervical cancer
25-65: Women and other individuals with a cervix at average risk for cervical cancer should start screening at age 25 and continue until at least age 65.
65+: You can stop screening at age 65 or older if you’ve been getting screened regularly and your last 2 HPV tests (or co-tests) or your last 3 Pap tests were normal.
Testing options:
A primary HPV test (HPV test alone) on a cervical sample collected by a health care provider every 5 years. This is the preferred option.
A primary HPV test done on a self-collected vaginal sample, every 3 years
A co-test (HPV test combined with a Pap test) every 5 years
A Pap test alone (if HPV testing isn't available) every 3 years
Endometrial cancer
The American Cancer Society recommends that at the time of menopause, all women should be told about the risks and symptoms of endometrial cancer. Women should report any unexpected vaginal bleeding or spotting to their doctors.
Some women – because of their history – may need to consider having a yearly endometrial biopsy. Please talk with a health care provider about your history.
Lung cancer
The American Cancer Society recommends yearly screening for lung cancer with a low-dose CT (LDCT) scan for people ages 50 to 80 who smoke or used to smoke and have at least a 20 pack-year history of smoking
A pack-year is equal to smoking 1 pack (or about 20 cigarettes) per day for a year. For example, a person could have a 20 pack-year history by smoking 1 pack a day for 20 years, or by smoking 2 packs a day for 10 years.
Colorectal cancer and polyps
45: Start regular screening
46-75: Continue regular screening if in good health
76-85: Talk with your health care provider about whether continuing to get screened is right for you. When deciding, take into account your own preferences, overall health, and past screening history.
85+: Should no longer get colorectal cancer screening.
Prostate cancer
Starting at age 50, men should talk to a health care provider about the pros and cons of testing so they can decide if testing is the right choice for them.
If you are African American or have a father or brother who had prostate cancer before age 65, you should have this talk with a health care provider starting at age 45.
If you decide to be tested, you should get a PSA blood test with or without a rectal exam. How often you’re tested will depend on your PSA level.